Menopause: How Will I Know?
- posted: Aug. 14, 2023
As women get older, menopause begins to approach, and it can feel daunting. The only thing that most people know about menopause is that it signifies the end of your Read More
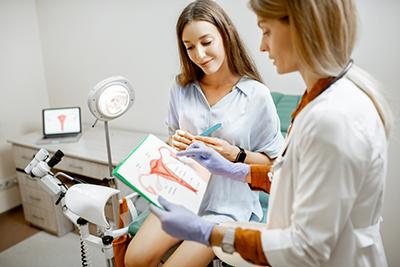
When To Visit an OBGYN
- posted: Aug. 01, 2023
An OBGYN is an expert in women's health. Annual routine visits to your OBGYN can help safeguard your reproductive health. Your OBGYN can tell you more. What You Need To Know Read More
Managing Menopause: Tips for a Smooth Transition
- posted: Jul. 18, 2023
As a woman ages, hormone levels will begin to drop, leading to a process known as menopause. Menopause happens when your period ends, and your body begins to adapt and Read More
Common Gynecological Conditions: Causes, Symptoms, and Treatment
- posted: Jul. 05, 2023
A gynecologist throughout different life stages is crucial for women's reproductive and overall health. These specialized doctors provide essential care, guidance, and support. A gynecologist can educate young women about Read More
When Should You See a GYN?
- posted: Jun. 22, 2023
If you are a woman, your reproductive health is critical at all stages of your life. Whether you are a teen experiencing puberty, a woman considering having children, or a Read More
Common Causes of Painful Periods
- posted: Jun. 05, 2023
Menstruation can vary widely between women. Some women have periods which are regular, and others have irregular or absent periods. Some women have periods which only last about three days, Read More
Common Gynecological Conditions and How to Treat Them
- posted: May 22, 2023
There are many issues that can affect the way that a woman’s body works, and it can cause pain and irritation throughout your life. Gynecological problems can also cause complications Read More
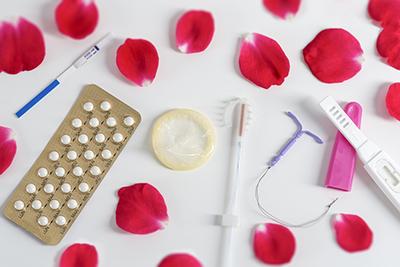
Questions to Ask Your GYN About Birth Control
- posted: May 08, 2023
When it comes to birth control, you have many options to choose from. It can be overwhelming to sift through all the information available about birth control. It’s important that Read More
The Importance of Regular Gynecological Exams for Women's Health
- posted: Apr. 13, 2023
When it comes to women’s health, there are specific needs that should be met. Gynecological exams help to make sure that everything is functioning properly and that there aren’t any Read More
Do I Need to Have a Pap Smear?
- posted: Apr. 10, 2023
Taking care of yourself also means taking preventive measures to ensure that any serious issues are dealt with as quickly as possible. One important measure that all women will need Read More
Women's Health: Essential Screenings and Preventive Care for Every Stage of Life
- posted: Mar. 24, 2023
For most sicknesses, we wish would have taken steps before getting sick, but can get over the illness quickly. There are some issues that aren’t as easy to treat and Read More
Understanding Reproductive Health: Common Conditions and Treatment Options
- posted: Mar. 15, 2023
Reproductive health is important and if women are struggling with untreated reproductive health issues, it can affect their daily lives. It’s important that you’re able to identify if you might Read More
What Can Cause Pelvic Pain?
- posted: Feb. 28, 2023
Dealing with pelvic pain can severely interrupt your normal routine. It can cause issues with your digestive, reproductive, or urinary system and can be incredibly disruptive. There are many issues Read More
The Benefits of Regular Gynecological Exams
- posted: Feb. 09, 2023
How often do you visit your gynecologist? If you don’t see your gynecologist at least once each year, you are missing out on an important way to protect your health. Read More
Navigating the Different Birth Control Options
- posted: Jan. 26, 2023
Having a baby is a wonderful experience, and it’s helpful to have a baby when you’ve planned on starting a family. Birth control can help prevent pregnancy, so you can Read More
The Importance of Regular Gynecological Exams
- posted: Jan. 12, 2023
Your reproductive health is important. Regular gynecological exams can help protect your reproductive health and help prevent serious medical conditions like cervical cancer. Your GYN doctor is dedicated to protecting Read More
Our Location
133 Falmouth Rd. 2A Suite A
Mashpee, MA 02649
(877) 669-1746